DAY 3 — “The Night I Finally Breathed.”
April 3rd, 2026 — Weight: 101.2kg. Walk: 7.64km. CPAP: 6 hours 42 minutes.
Last night something shifted.
I’ve recently discovered the benefits of positional therapy for sleep apnea, which has changed my perspective on managing this condition.
Not dramatically. Not perfectly. But genuinely, measurably, scientifically — something shifted.
Two nights ago I wore my CPAP mask for one hour and four minutes before my sleeping self staged its usual revolt and removed it. My blood oxygen dropped to 88%. The myAir app gave me a score of 41 out of 100 and suggested I seek support. It was, in the polite language of medical software, a failure.
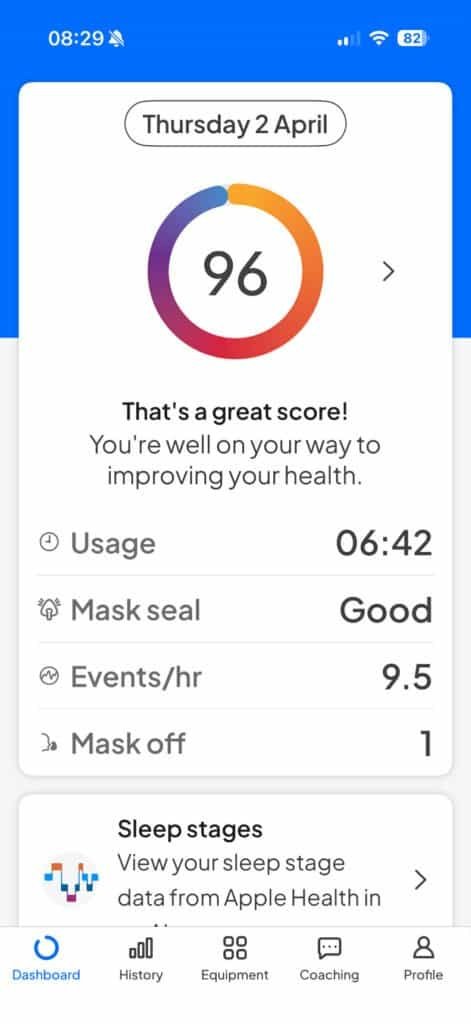
Last night I wore it for six hours and forty-two minutes.
This approach, known as positional therapy for sleep apnea, encourages sleeping in specific positions to reduce apnoeic events.
I’m hopeful that with continued practice of positional therapy for sleep apnea, I will see even more improvement.
The app gave me a score of 96 out of 100. It said: “That’s a great score. You’re well on your way to improving your health.”
I am choosing to believe it.
What Changed — And Why It Matters
Two things were different last night. First, I wore the positional sleep therapy vest for the first time — a lightweight device with a foam ball positioned between the shoulder blades that makes sleeping on your back physically uncomfortable, gently steering you onto your side throughout the night. Positional sleep apnea — where breathing events occur predominantly when lying on the back — is extraordinarily common, and side sleeping keeps the airway open passively without any equipment at all. The vest addresses the root cause. The CPAP treats the symptoms. Together, they are formidable.
Second, I was simply more determined. I tried to take the mask off three times during the night. Each time, the disturbance woke me just enough to notice — and I put it back on.
That is not a small thing. That is the difference between a score of 41 and a score of 96.
What “Sleep Duration” Actually Means — And Why My Devices Disagree
Before we look at last night’s sleep data, it is worth understanding why the Fitbit and the Hume Band report such different figures for the same night — because this is one of the most misunderstood aspects of consumer sleep tracking.
Fitbit reports time asleep. It uses movement and heart rate to identify every moment you were awake during the night and subtracts all of it from the total. Last night it logged 1 hour and 1 minute of awake time — and reported my sleep as 5 hours 58 minutes. That is not a flaw. That is Fitbit being precise about actual unconscious sleep time.
The Hume Band reports total sleep session length — the full duration from when you fell asleep to when you got up, including brief awakenings. It recorded 6 hours 59 minutes.
The CPAP machine, which has no opinion about sleep stages and simply measures mask usage time, recorded 6 hours 42 minutes. That figure sits precisely between the two wearables and confirms the Hume Band’s session length as the more credible measure of how long I was in bed with the machine on.
Going forward I will use the Hume Band figure as my primary sleep duration — while keeping the Fitbit’s awake time and sleep stage breakdown as the more granular data layer. Both are useful. They are just measuring different things.
Fitbit sleep data for reference:
- Total session: 23:05–06:05
- Time asleep: 5h 58m
- Sleep score: 80/100
- Awake: 1h 1m / REM: 1h 23m / Light: 3h 59m / Deep: 35 min
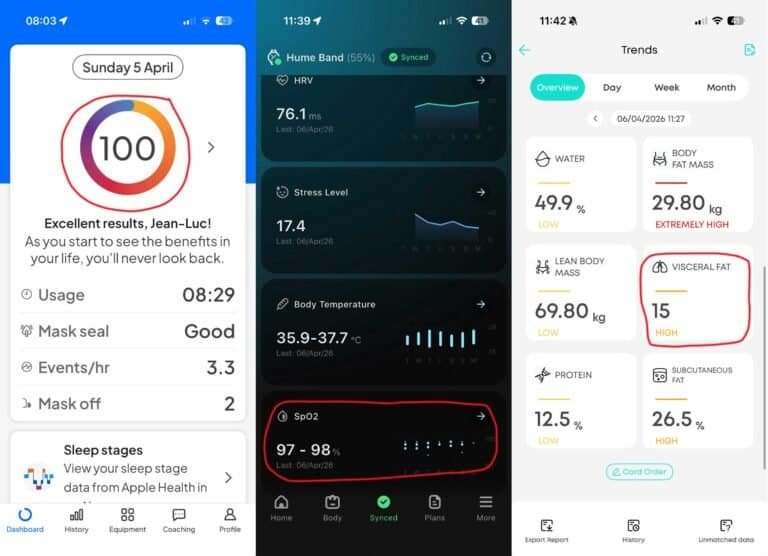
SpO2: From 88% to 95–98% — The Number That Changes Everything
Here is the headline from last night, and it is not a small one.
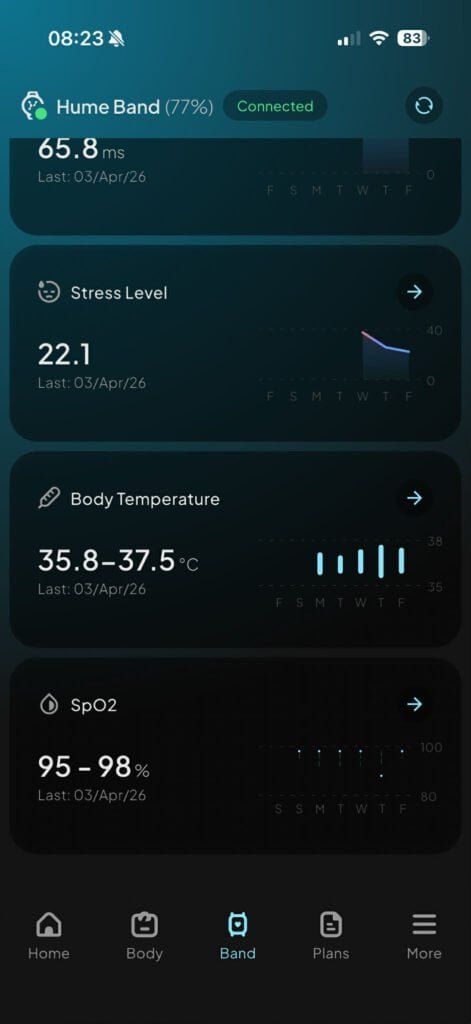
On Night 1, without adequate CPAP coverage, my blood oxygen dropped to 88% during sleep. Last night, with six hours and forty-two minutes of CPAP and the positional vest keeping me off my back, the Hume Band recorded my overnight SpO2 at 95–98%. Rated “High” — right where it should be.
| Night 1 | Night 3 | |
|---|---|---|
| CPAP usage | 1h 04m | 6h 42m |
| CPAP score | 41/100 | 96/100 |
| Events/hr | 0.9 (1 hour only) | 9.5 (treated, full night) |
| SpO2 overnight | 88% | 95–98% |
The events-per-hour figure of 9.5 deserves a moment of explanation, because it is higher than Night 1 and might look like a regression. It is not. On Night 1, I wore the mask for one hour during which my airway happened to be in a cooperative position — hence 0.9 events. On Night 3, I wore it for nearly seven hours, across all sleep stages and natural body movements. During that extended period the machine detected and actively treated 9.5 apnea events per hour. Clinically, an AHI between 5 and 15 is classified as mild sleep apnea. Untreated, mine is almost certainly moderate to severe. With the CPAP running for nearly seven hours, it was reduced to mild. That is the machine doing exactly what it costs £800 to do.
The oxygen data confirms it. 95–98% all night. No crashes. No hypoxemia. My organs got what they needed.
The positional vest is staying. The CPAP is staying. Both, together, every night.
Weight: What the Scales Say This Morning
- Eufy smart scales: 101.2 kg ⬇️ down 0.2 kg from yesterday
- Hume Pod: (body composition scan below — 102.3 kg)
A note on the Fitbit’s weight figure: it shows 101.2 kg, but this is simply the Eufy reading synced automatically via Apple Health. It is not an independent measurement, so I will not be citing it as a separate data point going forward. Eufy and Hume Pod are the two scales that matter in this series.
The Hume Pod weight has consistently read higher than the Eufy — it recorded 103.4 kg on Day 1 when Eufy showed 102 kg. This two-kilogram discrepancy is consistent and unexplained. I will be tracking both figures daily and asking Hume about their calibration methodology.
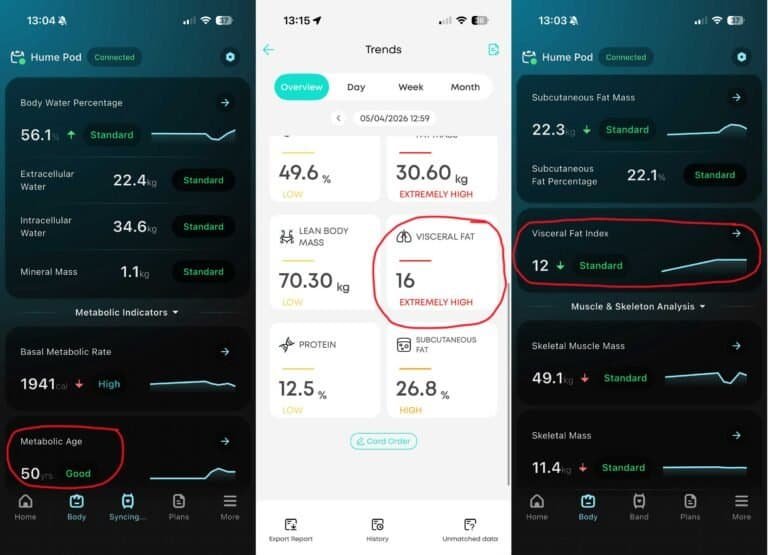
The Hume Pod Body Composition This Morning
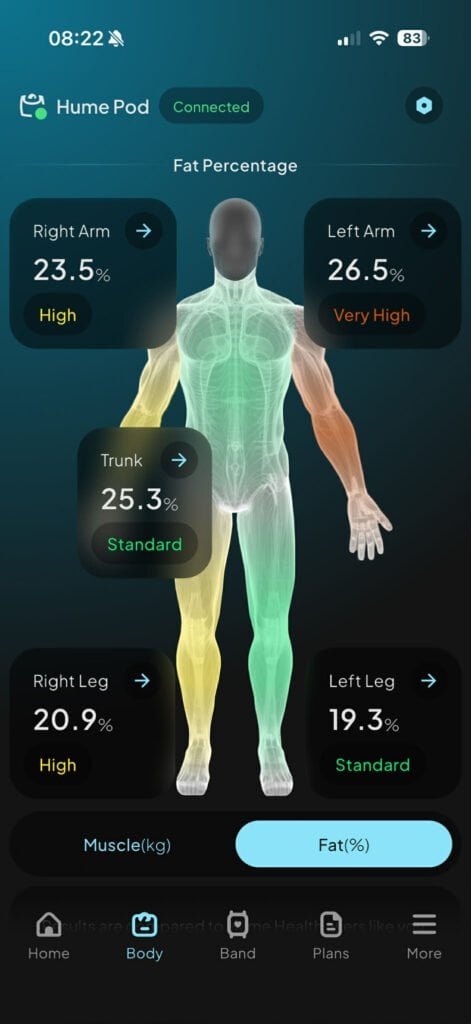
The Hume Pod scan today produced its most varied reading so far:
- Right Arm: 23.5% — High
- Left Arm: 26.5% — Very High (first “Very High” reading in the series)
- Trunk: 25.3% — Standard (the belly, unmoved)
- Right Leg: 20.9% — High
- Left Leg: 19.3% — Standard
The left arm jumping to “Very High” is worth noting. This is my non-dominant arm and it did the same walking work as the right this morning. My instinct is that this reading reflects post-exercise fluid distribution rather than genuine overnight fat change — but it is exactly the kind of day-to-day volatility that raises questions about how much weight to give individual Hume Pod readings versus trends over time.
The trunk remains “Standard” despite the Eufy confirming visceral fat of 16 — Extremely High — for the third consecutive day. More on this below.
Hume Replied — And Revealed Something Important
Yesterday Hume Support confirmed what “users like you” actually means as a benchmark:
“Your Visceral fat rating and other body composition metrics are scored against established benchmarks specifically for people of your same age, sex at birth, and height.”
Age. Sex at birth. Height.
Not weight.
If the benchmark cohort for a 55-year-old man at 189cm includes both lean athletic men and those carrying significant excess weight — because the only filters are age, sex and height — then “Standard” simply means somewhere in the middle of all tall 55-year-old men. It does not mean clinically healthy. It means not an outlier in a mixed population.
Meanwhile the Eufy scales, which benchmark against clinical health thresholds rather than peer groups, have called my visceral fat Extremely High every single day.
I have sent Hume a follow-up question: does the benchmark cohort include weight, and which clinical database underpins their thresholds? I will publish their reply in full when it arrives.
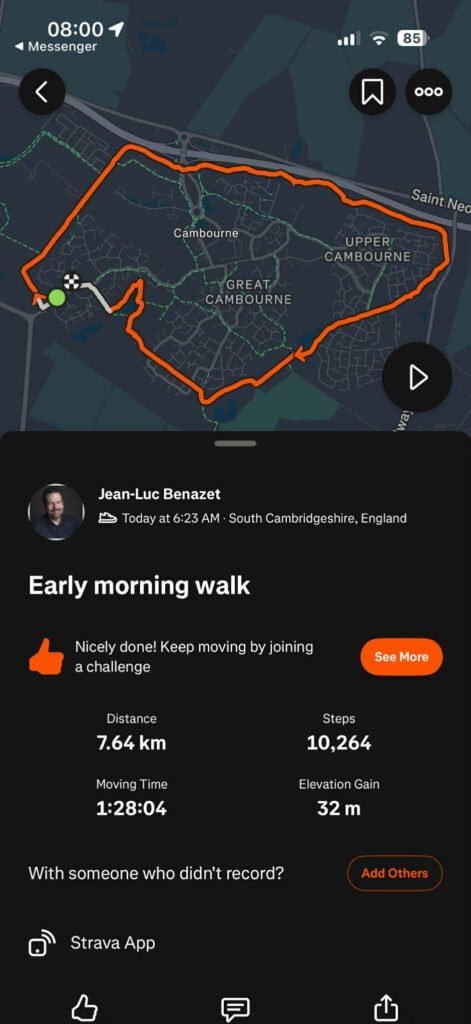
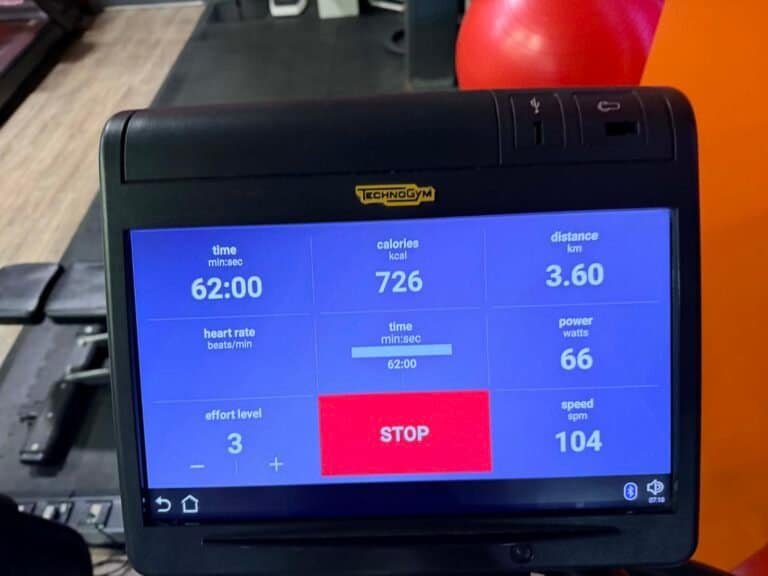
No Gym Today — But 7.64km Before Breakfast
The gym does not open until 8am on bank holidays. Rather than wait, I was out of the door at 6:23am for an early morning walk around Cambourne in South Cambridgeshire. One hour twenty-eight minutes. 7.64 kilometres. 10,264 steps. Thirty-two metres of elevation gain.
I finished with five minutes of stretching.
There is something particular about walking before the world starts. The kind of quiet that makes it slightly easier to have an honest conversation with yourself about where you are and where you are going.
My left knee, however, had strong opinions.
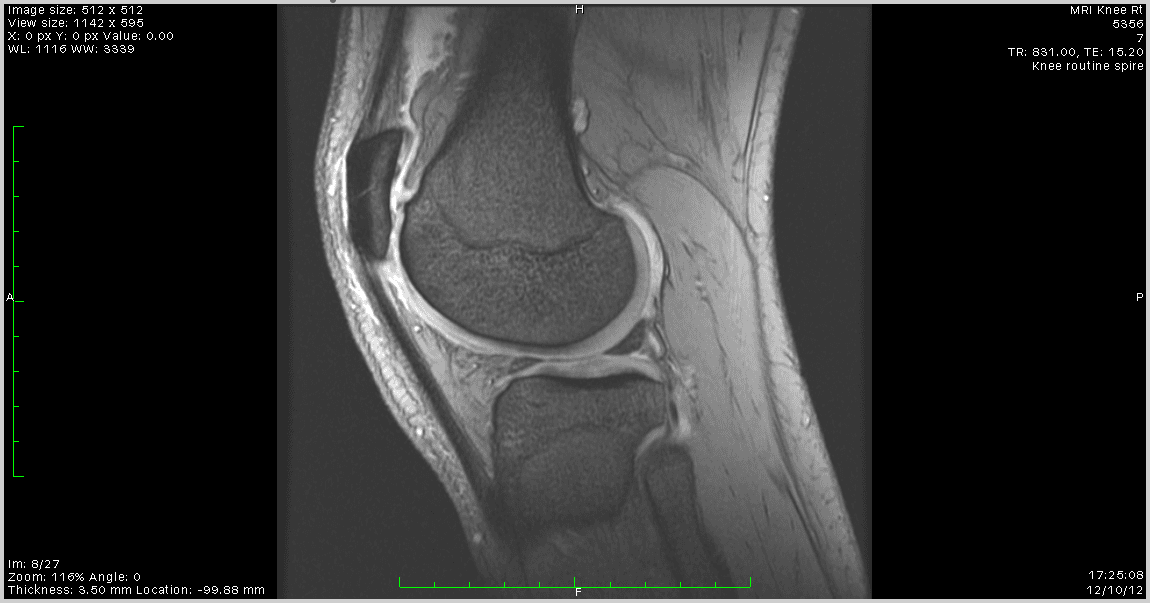
It seized several times during the walk — a grinding reluctance from a joint that has been carrying too much weight for too long. This is not new. I have been warned that arthritis may be developing in both knees. An MRI of my right knee from 2012 showed early structural changes consistent with excess load over time. I have included that scan here not for drama but for context: this is what carrying 101 kilograms looks like from the inside, a decade and a half of it.
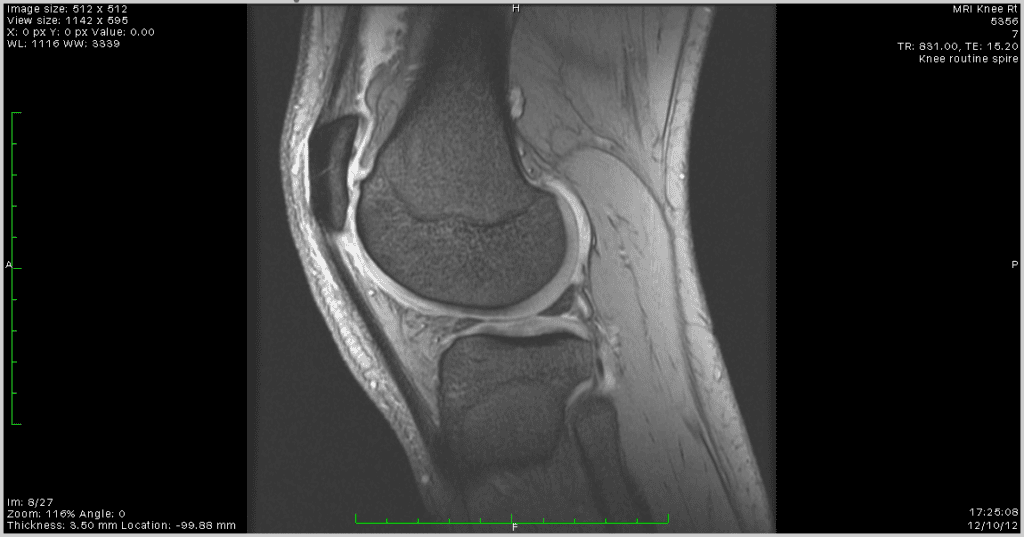
Every kilogram I lose between now and Day 30 is a kilogram that knee no longer has to support. The target of 88 kilograms is not an aesthetic goal. It is a medical one.
Today’s Special Circumstances: A Wedding
This afternoon I am at a wedding as a guest. Suit, ceremony, reception, champagne within arm’s reach at all times. I am driving, which resolves the alcohol question without requiring any particular virtue on my part. No alcohol today. I will take the win regardless of the mechanism.
Intermittent fasting continues. Eating window from midday. Real food at the reception, not a free-for-all.
The vest and the CPAP will be on tonight. Non-negotiable.
Day 3 Summary
| Metric | Value | Direction |
|---|---|---|
| Weight (Eufy) | 101.2 kg | ⬇️ -0.2 kg |
| Morning walk | 7.64 km / 1h 28m | ✅ |
| Steps (Hume Band) | 10,937 | ✅ |
| Steps (Fitbit) | 10,645 | ✅ |
| Sleep session (Hume Band) | 6h 59m | ✅ |
| Time asleep (Fitbit) | 5h 58m | ✅ (excl. awake) |
| CPAP usage | 6h 42m | ✅ Major improvement |
| CPAP score | 96/100 | ✅ |
| SpO2 overnight | 95–98% | ✅ vs 88% Night 1 |
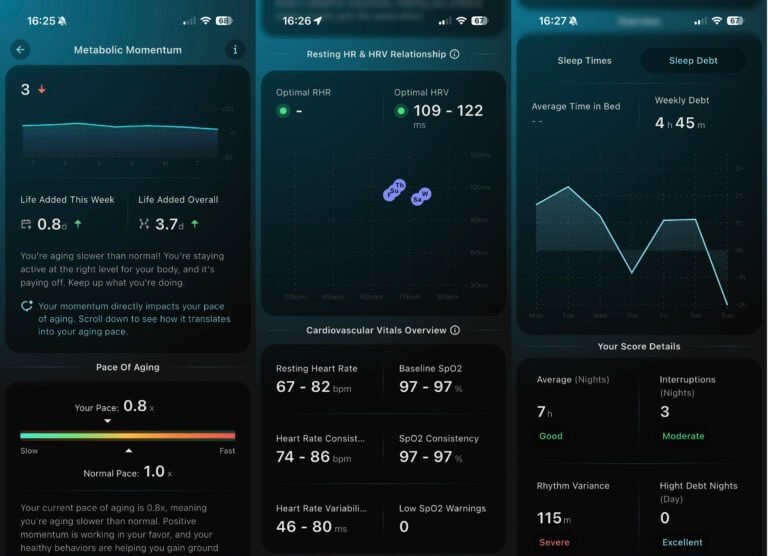
| Stress (Hume Band) | 22.1 | ⬇️ Improving |
| HRV | 65.8 ms | ➡️ Stable |
| Alcohol | 0 | ✅ |
Three days in. The weight is moving in the right direction. The oxygen is where it should be for the first time in who knows how long. The knee has filed a formal complaint.
Tonight: suit, wedding, water, early night, CPAP, vest.
— Day 3 of 30